Performance data
Ultravision™ has undergone a variety of rigorous independent tests, achieving outstanding results.
Ultravision consistently meets its primary objective of providing a clear visual field. Unlike some of its competitors, Ultravision’s technology ensures other ‘knock on’ effects are avoided, allowing it to achieve exceptional all-round results.
The below data highlights the ‘game-changing’ results achieved by Ultravision when measuring visualisation, surgical smoke management, CO2 management, and the procedural efficiencies achieved.
Visualisation performance data
Ultravision consistently delivers advanced visualisation,
optimising procedural performance
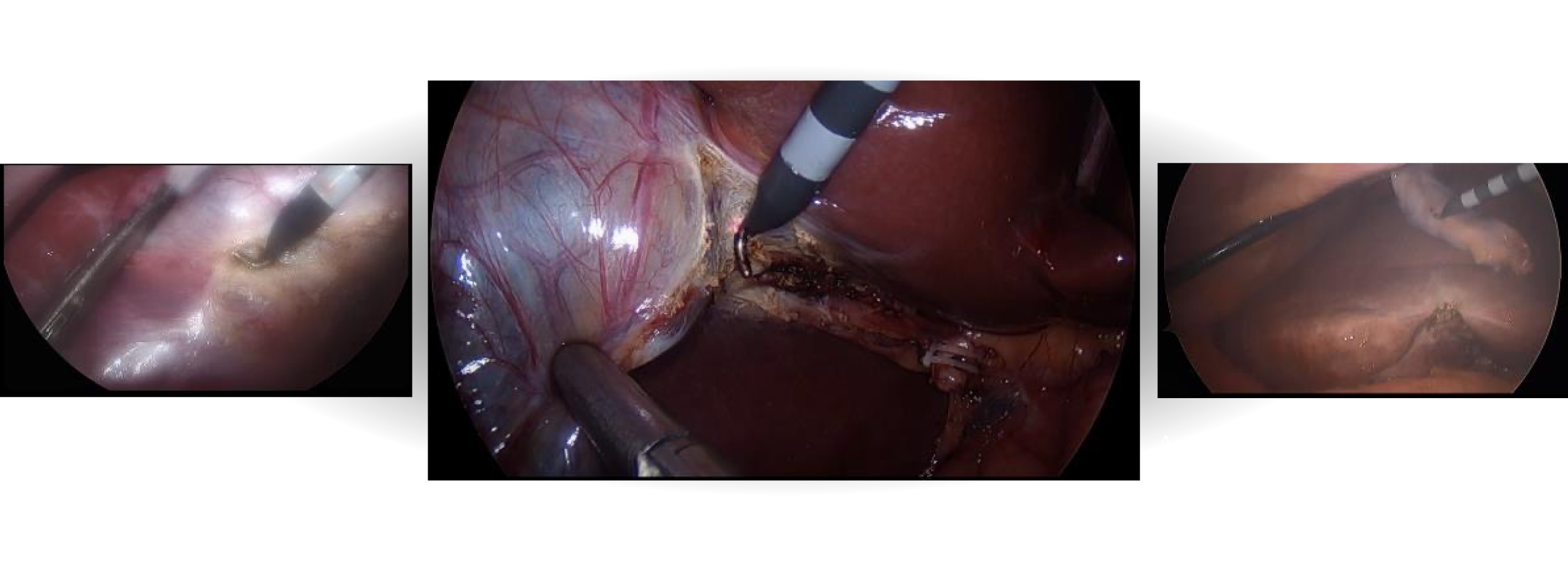
Visual field comparison
performed by Dr. Jin S. Yoo at
the Duke Regional Hospital, US
1) Rapidly suppresses surgical smoke which provides continuously clear visualisation
2) Ultravision does not rely on diluting the smoke filled abdomen with new CO2
3) Stable pneumoperitoneum due to no gas exchange facilitates low pressure, low flow surgery
Advanced visualisation study
Evaluate Ultravision's performance during laparoscopic cholecystectomy
Ansell et al (2014)
Test concluded that Ultravision improves
visibility during laparoscopic surgery and
significantly reduces procedural delays
for smoke clearing and camera cleaning.
The surgeon’s view
When we’re doing laparoscopic surgery visualisation is just about everything.
We need to be able see very clearly what we are doing and anatomically what we are trying to accomplish.
Dr. Richard Rosenfield, MD
Executive Medical Director
Pearl Women’s Center, US
Smoke management performance data
Ultravision proves to be more efficient in controlling bioaerosols than traditional smoke evacuation systems
Ultravision versus Continuous Smoke Evacuation Systems
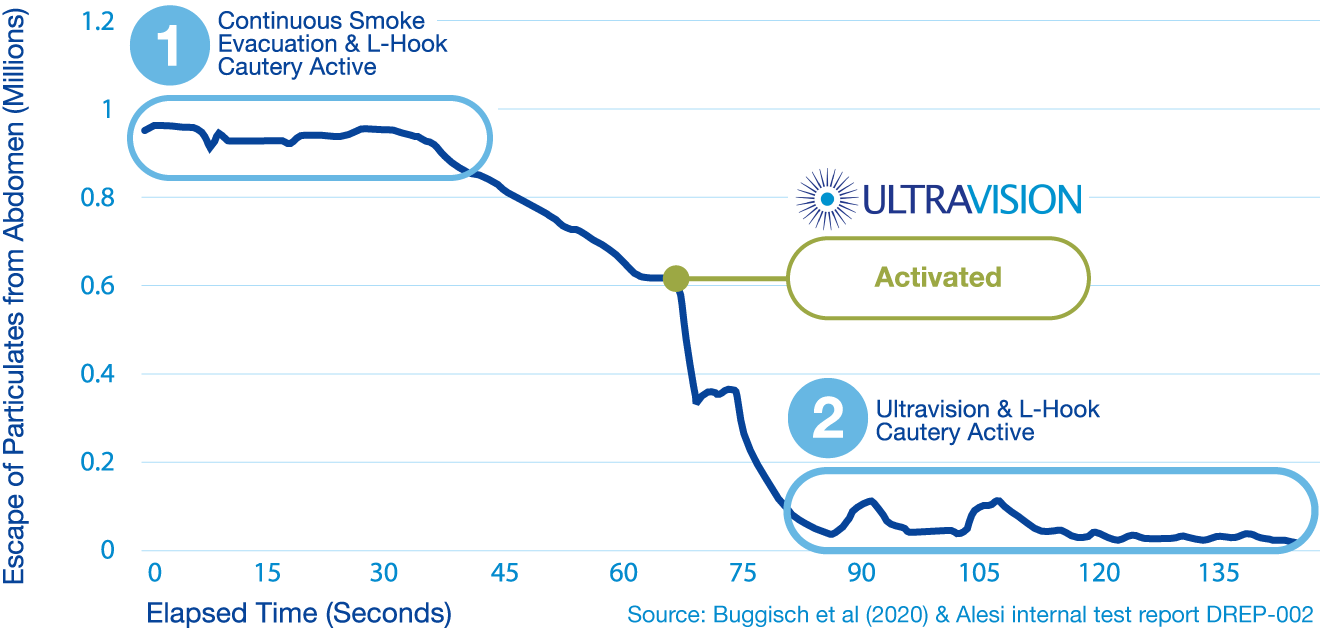
1) Continuous Smoke Evacuation experiences additional escape of smoke particulates through leaks in trocars and instruments exchanges.
2) Ultravision suppresses smoke and bioaerosols at the point of creation which reduces the likelihood of release in the operating room.
Bioaerosol escape from the abdomen into the Operating Room is significantly reduced with Ultravision.
A remarkable 23x reduction in bioaerosols is achieved.
Measuring speed & effectiveness. Ultravision v filter-based smoke evacuation system
Ultravision minimises surgical smoke, providing two levels of risk reduction;
Two levels of risk reduction
1. Particle suppression at the point of creation
2. More rapid elimination of smoke compared to smoke evacuators
After 60 seconds Ultravision removes 99.9% of particles from the atmosphere, versus 30.2% with a smoke evacuator.
Removal efficiency test for sub-viral particulates
1. Suppresses 99% of particulates down to 0.007um (7nm, sub-viral sized) from aerosolisation. Ability to contain sub-viral sized particles.
2. The only product independently verified to be effective at sub-viral particle sizes.
CO2 management performance data
Ultravision’s unique system facilitates low pressure, low flow surgery and reduces CO2 usage
A test to explore the use of Ultravision in facilitating low pressure surgery in total laparoscopic hysterectomy (TLH) and myomectomy.
Ultravision enhances low pressure laparoscopic hysterectomy and myomectomy. This was achieved by minimizing interruptions to surgery and exchange of CO2; providing a clear visual field throughout the procedure; and eliminating surgical smoke at the site of origin.
Source: Levine et al (2020)
Dr. Jin S. Yoo demonstrates the benefits of Ultravision
when performing Bariatric surgery Roux-en-Y.
A clear field of view is maintained
alongside a stable pneumoperitoneum.
Dr Yera and Mr Misra share their experience of
using Ultravision in laparoscopic surgery.
CO2 pressure is maintained due to low exchange of CO2.
Low volume CO2 used, resulting in a high level of surgeon satisfaction in being able to operate at the lowest safe pressure whilst using minimal CO2, in line with clinical guidelines.
Improving OR efficiency
Ultravision enables a more efficient OR through time savings and reduced CO2 usage.
Oxford University Hospitals measured the procedural efficiencies achieved across four laparoscopic specialties.
The financial impact was calculated based upon any efficiency gain.
*Source: Efficiency and Innovation presentation given at the HCSA conference, 2017.
Efficiency improvements in all specialties:
- Gynae - 20 minutes per procedure
- Upper GI - 14 minutes per procedure
- Colorectal - 10 minutes per procedure
- Urology - 9 minutes per procedure
- Potential to add 1 additional procedure per list
plus reduced risk of overrun
An additional £1.7m revenue per year was estimated, based upon the ability to schedule additional procedures.
Evaluate Ultravision performance during laparoscopic cholecystectomy
- 8 minutes per case saved
- Zero pauses in 77% of procedures
- No camera cleaning required in 95% of cases
Prevents Smoke
Release into OR
Improves
Visibility
Reduces
Camera Cleaning
Reduces Pauses
During Procedure
Facilitates Low
Pressure Surgery
Reduces CO2
Consumption
*1 ‘Advanced Visualisation Study’ Ansell 2014 (Ansell et al, Electrostatic precipitation is a novel way of maintaining visual field clarity during laparoscopic surgery: a prospective double-blind randomised controlled pilot study Surgical Endoscopy (2014) 28: 2057-2065).
*2 ‘Smoke Management Performance Data’ Buggisch 2020 ( Buggisch et al, Experimental Model to Test Electrostatic Precipitation Technology in the COVID-19 Era: A Pilot Study Journal of American College of Surgeons, (2020), 231 (6) 704-712).
*3 ‘UV vs. filter-based smoke evac’ DREP report 2012 (Based on internal validation - DREP 002 (2012) A Study Of The Ability Of The Ultravision Electrostatic Precipitator To Clear The Particulate Matter Produced By Energy-Based Surgical Instruments).
*4 ‘CO2 Management Performance’ Levine 2020 (Levine, D et al, “Electrostatic Precipitation in Low Pressure Laparoscopic Hysterectomy and Myomectomy” (2020), JSLS, Volume 24, Issue 4).
